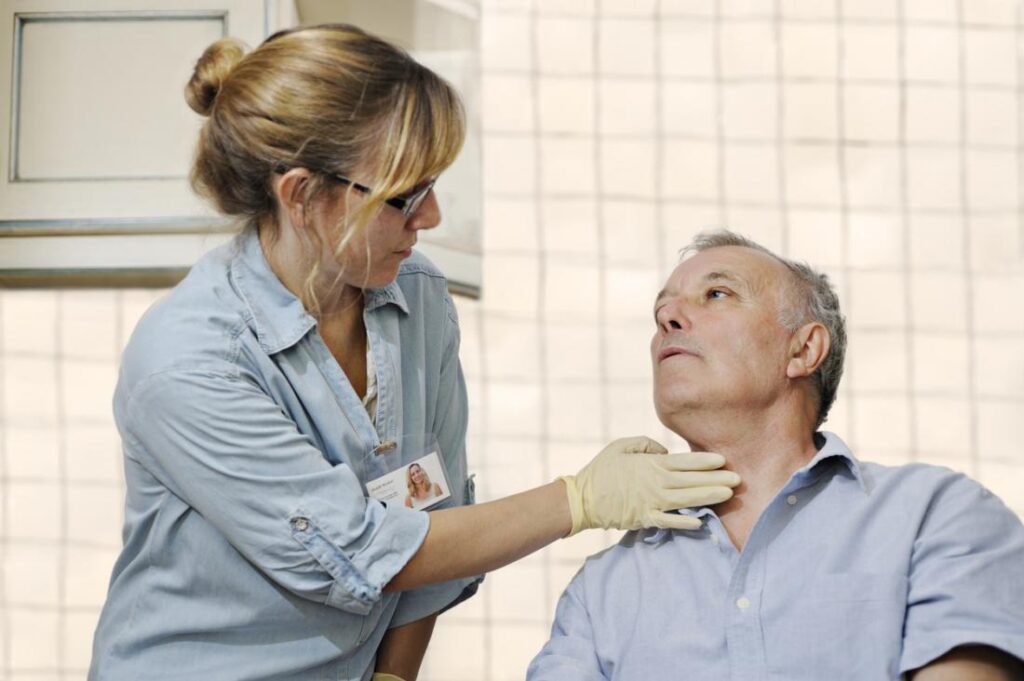
In the world of care work, there are moments that carry more weight than others. Assisting someone with medication, supporting mobility, responding to an emergency — these are all critical responsibilities. But there is one everyday activity that is often underestimated in its risk: eating and drinking.
For individuals living with dysphagia, swallowing is not automatic. It is a complex, fragile process that can quickly become life-threatening without the right support. A single bite of food or sip of fluid can trigger choking, aspiration or serious medical complications if care is not delivered correctly.
This is why dysphagia support training in Australia has become a vital component of both NDIS and aged care practice. It is not simply about feeding someone — it is about protecting their airway, preserving their dignity, and ensuring their ongoing health and wellbeing.
In this article, we explore the importance of dysphagia support training, what it involves, the risks of inadequate care, and why accredited NDIS training is essential for anyone working in the Australian healthcare sector.

Key Takeaways
- Dysphagia support is one of the most critical — and often underestimated — responsibilities in the care sector. It requires a combination of clinical knowledge, practical skill and compassionate care.
- As the Valmar case demonstrates, the consequences of getting it wrong can be severe. But with proper training, these risks can be significantly reduced.
- For NDIS and aged care workers in Adelaide, dysphagia support training is not just a professional development opportunity — it is an essential safeguard for the people they support.
What Is Dysphagia? Understanding Swallowing Difficulties in Australian Care Settings
Dysphagia is the clinical term used to describe difficulty swallowing. While this may sound straightforward, swallowing itself is a highly coordinated action involving multiple muscles and nerves working in precise sequence. When that coordination is disrupted, the consequences can be significant.
Dysphagia can affect people of all ages, but it is particularly common among:
- Older adults in residential aged care
- People recovering from stroke
- Individuals with neurological conditions such as Parkinson’s disease or multiple sclerosis
- NDIS participants with complex physical or cognitive disabilities
For these individuals, swallowing difficulties may present as coughing during meals, difficulty chewing, prolonged eating times or avoidance of certain foods. In more severe cases, food or fluid can enter the airway instead of the oesophagus — a process known as aspiration.
What makes dysphagia especially dangerous is that it is often progressive and sometimes silent. A person may not always show obvious signs of distress, even when aspiration is occurring. This is why trained observation and intervention are so important.
From a care perspective, dysphagia is not just a medical condition — it is a high-risk daily activity that must be managed with precision and consistency.

Why Dysphagia Support Training Is Critical for NDIS and Aged Care Workers in Adelaide
Across both the NDIS and aged care sectors, there is a growing recognition that dysphagia support is a specialised skill — not a general care task.
Under the NDIS Practice Standards, dysphagia falls within High Intensity Daily Personal Activities (HIDPA). This classification reflects the level of risk involved and the need for workers to demonstrate competency before providing support.
In practical terms, this means that support workers are expected to:
- Understand and follow individualised dysphagia support plans
- Apply safe feeding and positioning techniques
- Recognise early signs of swallowing difficulty or deterioration
- Respond appropriately to choking or airway emergencies
Without proper training, even well-intentioned care can become unsafe. A worker may unknowingly provide food of the wrong texture, rush a meal, or position a client incorrectly — all of which can increase the risk of aspiration or choking.
As regulatory frameworks evolve in Australia, there is also increasing accountability placed on providers. Dysphagia support training is no longer just encouraged — it is expected.

The Real Risks of Poor Dysphagia Management: More Than Just Choking
When dysphagia is not managed correctly, the risks extend far beyond a single choking incident.
At the most immediate level, there is the risk of airway obstruction, where food blocks the airway and prevents breathing. This can lead to loss of consciousness and cardiac arrest within minutes.
However, one of the most serious and often overlooked risks is aspiration pneumonia. This occurs when food, fluid or saliva enters the lungs, leading to infection. It is a leading cause of hospitalisation and death among vulnerable populations.
There are also longer-term health consequences. Individuals with dysphagia may avoid eating or drinking due to fear or discomfort, resulting in malnutrition and dehydration. Over time, this can lead to weight loss, reduced immunity, fatigue and a general decline in health.
These risks are compounded when care is inconsistent or when staff are not adequately trained. Dysphagia management requires precision, patience and vigilance — qualities that are developed through structured, accredited training and supervised practice.

Case Study: The Valmar Incident — A Preventable Tragedy
In 2025, a landmark case in Australia brought national attention to the importance of dysphagia support training. An NDIS provider, Valmar Support Services, was fined approximately $1.9 million following the death of a participant who choked during a meal.
The circumstances of the case were both confronting and instructive.
The participant had known swallowing difficulties and a documented dysphagia management plan. This plan specified the type of food that could be safely consumed and the level of supervision required during meals.
However, the investigation revealed that these guidelines were not followed. The individual was provided with food that did not meet the prescribed texture requirements, and staff lacked the training needed to recognise and manage the risks involved.
The outcome was a fatal choking incident — one that the court determined was preventable.
This case serves as a powerful reminder that dysphagia support is about a suite of responsibilities: HIPDA competence, compliance, accountability and duty of care. It also highlights the consequences of failing to provide staff with the accredited training they need to perform their roles safely.

What You Learn in Dysphagia Support Training for Support Workers
A comprehensive dysphagia support training course is designed to bridge the gap between theory and practice. It equips workers with the knowledge and skills required to provide safe, effective and person-centred care.
At its core, the training focuses on understanding swallowing and recognising when something is not right. Participants learn to identify early warning signs such as coughing, throat clearing, changes in voice quality and difficulty managing food.
From there, the training moves into practical application. One of the most important components is safe feeding technique. This includes pacing, portion control and ensuring that the individual is positioned correctly — typically upright and well-supported.
Another key area is the use of texture-modified diets. In Australia, this is guided by the International Dysphagia Diet Standardisation Initiative (IDDSI), which provides a framework for categorising food and fluid consistency.
IDDSI Framework Overview
A simple guide to common texture and fluid levels used in dysphagia support to help promote safer swallowing and more consistent mealtime care.
Providing the wrong texture — even unintentionally — can significantly increase the risk of choking. Training ensures that workers understand how to prepare, identify and deliver the correct consistency.
Importantly, dysphagia training also includes choking first aid. Workers are taught how to recognise airway obstruction and respond quickly and appropriately, using established first aid principles.

Mealtime Management: Where Safety and Dignity Meet
Mealtimes are more than just a functional activity — they are a deeply social and personal experience. For individuals with dysphagia, however, mealtimes can become a source of anxiety.
This is where mealtime management plans play a crucial role. These plans outline exactly how a person should be supported during eating and drinking, including:
- Approved food and fluid textures
- Required level of supervision
- Positioning and feeding techniques
- Environmental considerations
Following these plans is not optional — it is essential for safety.
At the same time, good dysphagia care must also respect the individual’s dignity and preferences. This means allowing choice where possible, maintaining a calm and supportive environment, and avoiding practices that may feel rushed or impersonal.
Balancing safety with dignity is one of the defining skills of a well-trained support worker.
Monitoring, Reporting and Team-Based Care
Dysphagia support does not occur in isolation. It is part of a broader care framework involving multiple professionals, including speech pathologists, nurses and care coordinators.
Support workers are often the first to notice changes in a person’s swallowing ability. This makes their role in monitoring and reporting especially important.
Small changes — such as increased coughing, longer meal times or reduced appetite — can signal a deterioration in swallowing function. Prompt reporting allows for timely reassessment and adjustment of care plans.
Training emphasises the importance of accurate documentation, clear communication and collaboration with the wider care team. These are not just administrative tasks — they are critical components of safe care.

Equipment and Aids in Dysphagia Support
In many cases, specialised equipment is used to support safe eating and drinking. This may include modified utensils, adaptive cups, thickening agents and positioning supports.
While these tools can be highly effective, they must be used correctly. Improper use can reduce their effectiveness or even introduce new risks.
Training ensures that workers understand:
- When to use specific aids
- How to maintain hygiene and safety
- How to support independence while ensuring safety
Why Accredited Dysphagia Support Training Matters
In an increasingly regulated care environment, accredited training provides assurance — for workers, providers and clients alike.
For workers, it builds confidence and competence. It allows them to approach mealtime support with clarity, rather than uncertainty.
For providers, it demonstrates compliance with NDIS Practice Standards and reduces the risk of incidents and legal consequences.
For clients, it ensures that they receive care that is not only safe, but also respectful and person-centred.
Accredited Dysphagia Support Training is not just about meeting requirements — it is about raising the standard of care.
Safe Dysphagia Support Principles
These essential principles help promote safer swallowing, more consistent mealtime care and better outcomes for people requiring dysphagia support.
Follow the care plan exactly
Always follow the person’s current dysphagia support plan and approved mealtime instructions without making assumptions or substitutions.
Use correct IDDSI food and fluid textures
Provide only the prescribed food texture and fluid consistency to reduce the risk of choking, aspiration and unsafe swallowing.
Ensure upright positioning
Support the person to sit upright and comfortably during meals so swallowing can occur as safely and effectively as possible.
Provide calm, unhurried mealtime support
Create a quiet, supportive environment and allow enough time for each mouthful so the person does not feel rushed or distressed.
Monitor continuously for signs of difficulty
Watch closely for coughing, throat clearing, wet voice, fatigue, distress or any change in swallowing ability during meals and drinks.
Be prepared to respond to choking
Know the choking response procedures, stay alert throughout mealtimes and act promptly if the person shows signs of airway obstruction.
Report any changes immediately
Escalate and document any changes in swallowing, eating, drinking or mealtime tolerance so the care team can review support needs promptly.
Knowledge Test: Dysphagia Support Quiz
Test your understanding of dysphagia support, choking risk and IDDSI principles with this quick interactive quiz.
References
- NDIS Practice Standards and Quality Indicators
- International Dysphagia Diet Standardisation Initiative (IDDSI)
- Speech Pathology Australia – Dysphagia Guidelines
- Australian Commission on Safety and Quality in Health Care
- Federal Court of Australia – Valmar Support Services Case
Frequently Asked Questions
What is dysphagia support training in Australia?
It is specialised training that teaches support workers how to safely assist individuals with swallowing difficulties, including feeding techniques, texture-modified diets and emergency response.
Is dysphagia a high intensity support under the NDIS?
Yes. It is classified under High Intensity Daily Personal Activities, requiring workers to be trained and assessed as competent.
What are the risks of poor dysphagia care?
Choking, aspiration pneumonia, malnutrition and potentially fatal outcomes.
What is the IDDSI framework?
A global standard used in Australia to classify food and fluid textures for safe swallowing.
Do aged care workers need dysphagia training?
Yes. It is essential for safe practice, compliance and quality care.